2026 Medicare vs. Medicaid: Coverage Comparison & Updates

Comparing 2026 Medicare and Medicaid Updates: Which Program Offers Better Coverage for Your Needs?
Understanding the intricacies of healthcare coverage can be a daunting task, especially when trying to differentiate between major government programs like Medicare and Medicaid. As we look ahead to 2026, it’s crucial to be informed about the latest updates, eligibility requirements, and the specific benefits each program offers. For many, the choice or combination of these programs can significantly impact access to vital medical services. This comprehensive guide aims to demystify the Medicare Medicaid 2026 landscape, providing a clear comparison to help you determine which program, or combination, is best suited for your individual or family’s healthcare needs.
Both Medicare and Medicaid are foundational pillars of the American healthcare system, designed to provide health insurance to specific populations. However, their target demographics, funding structures, and covered services differ significantly. While Medicare primarily serves individuals aged 65 or older, younger people with certain disabilities, and those with End-Stage Renal Disease (ESRD) or Amyotrophic Lateral Sclerosis (ALS), Medicaid is a state and federal program that provides healthcare coverage to low-income individuals and families. The upcoming 2026 updates are poised to bring shifts in policy, costs, and availability, making it more important than ever to stay informed.
This article will delve into the core aspects of each program, including their eligibility criteria, the range of services they cover, typical out-of-pocket costs, and how they interact with each other. We will also highlight any anticipated changes for 2026, offering proactive insights into potential impacts on beneficiaries. Whether you are approaching eligibility age, managing a disability, or seeking assistance for low-income healthcare, a thorough understanding of Medicare Medicaid 2026 is essential for making informed decisions about your health and financial well-being.
Understanding Medicare: Eligibility, Parts, and 2026 Outlook
Medicare is a federal health insurance program primarily for people aged 65 or older, but also for certain younger people with disabilities and individuals with specific medical conditions. To fully grasp its offerings, it’s important to understand its different parts.
Medicare Part A: Hospital Insurance
Part A covers inpatient hospital stays, care in a skilled nursing facility, hospice care, and some home health care. Most people don’t pay a monthly premium for Part A if they or their spouse paid Medicare taxes through employment for a specified period. For 2026, we anticipate continued focus on hospital reimbursement models, potentially adjusting for inflation and quality-of-care metrics. Beneficiaries should monitor for changes in deductibles and co-insurance for extended hospital or skilled nursing stays, which are subject to annual adjustments to reflect healthcare costs.
Medicare Part B: Medical Insurance
Part B covers certain doctors’ services, outpatient care, medical supplies, and preventive services. Most people pay a monthly premium for Part B, which can be deducted from their Social Security benefits. The premium amount, deductibles, and co-insurance rates are typically announced towards the end of the preceding year. For 2026, expect adjustments based on healthcare spending trends and potentially new covered preventive services or therapies, reflecting advancements in medical science. The government continually evaluates new treatments for inclusion, and beneficiaries should keep an eye on official Medicare announcements for specific additions or changes to covered services under Part B.
Medicare Part C: Medicare Advantage Plans
Medicare Part C, also known as Medicare Advantage, is an alternative way to receive your Medicare benefits. These plans are offered by private companies approved by Medicare and include all the benefits and services covered under Parts A and B. Most Medicare Advantage Plans also offer extra benefits not covered by Original Medicare, such as vision, hearing, dental, and even prescription drug coverage. For 2026, the competitive landscape of Medicare Advantage is expected to continue to grow, with more plans offering tailored benefits and potentially lower out-of-pocket costs in certain areas. Beneficiaries should review plan offerings carefully during the annual enrollment period, as benefits, service areas, and provider networks can change year-to-year. The Centers for Medicare & Medicaid Services (CMS) is likely to continue its efforts to enhance plan transparency and consumer choice, ensuring that beneficiaries can make informed decisions when selecting a Medicare Advantage plan.
Medicare Part D: Prescription Drug Coverage
Part D adds prescription drug coverage to Original Medicare, some Medicare Cost Plans, some Medicare Private-Fee-for-Service Plans, and Medicare Medical Savings Account Plans. These plans are offered by private companies approved by Medicare. The cost and specific drugs covered vary significantly between plans. For 2026, there may be further implementation of policies aimed at lowering drug costs, such as price negotiation provisions or caps on out-of-pocket spending for certain medications. These changes could significantly benefit beneficiaries, especially those with high prescription drug expenses. Staying informed about the formulary (list of covered drugs) and cost-sharing structures of different Part D plans will be crucial. The federal government’s ongoing initiatives to control prescription drug prices could lead to more affordable options for seniors and individuals with disabilities, making the Medicare Medicaid 2026 comparison even more relevant.
Projected 2026 Medicare Updates
While specific figures for 2026 are not yet finalized, historical trends suggest incremental increases in premiums, deductibles, and co-insurance for Parts A and B. Policy discussions often revolve around the solvency of the Medicare trust fund, drug pricing, and expanding access to innovative treatments. Beneficiaries should prepare for potential adjustments in out-of-pocket costs and monitor for any legislative changes that could affect their coverage. The focus remains on ensuring the sustainability of the program while adapting to the evolving healthcare landscape. For those planning their retirement or managing existing health conditions, understanding these potential shifts in Medicare Medicaid 2026 is paramount.
Delving into Medicaid: Eligibility, Benefits, and 2026 Outlook
Medicaid is a joint federal and state program that provides health coverage to millions of Americans, including eligible low-income adults, children, pregnant women, elderly adults, and people with disabilities. Unlike Medicare, which has largely uniform eligibility rules across states (with some variations for Medicare Advantage), Medicaid eligibility and benefits can vary significantly from state to state due to its federal-state partnership structure.
Medicaid Eligibility Criteria
Eligibility for Medicaid is primarily based on income and family size relative to the Federal Poverty Level (FPL). States that have expanded Medicaid under the Affordable Care Act (ACA) cover nearly all adults with incomes up to 138% of the FPL. In states that have not expanded, eligibility for adults is much more restrictive. Children and pregnant women generally have higher income thresholds for eligibility. Additionally, individuals who receive Supplemental Security Income (SSI) are typically automatically eligible for Medicaid in most states. For 2026, ongoing debates about federal funding for Medicaid expansion and the future of the ACA could influence eligibility rules in various states. It’s essential for individuals to check their specific state’s Medicaid guidelines, as these can be updated annually.
Medicaid Covered Services
Medicaid provides a comprehensive set of benefits, often referred to as ‘Early and Periodic Screening, Diagnostic, and Treatment’ (EPSDT) services for children, and a broad range of services for adults. These generally include doctor visits, hospital stays, long-term care services, prescription drugs, mental health services, and transportation to medical appointments. Many states also offer additional benefits, such as dental and vision care, which are not typically covered by Original Medicare. For 2026, states may continue to innovate in how they deliver care, potentially expanding access to home and community-based services (HCBS) to reduce institutional care, or increasing coverage for telehealth services. The scope and depth of Medicaid benefits are a crucial aspect when comparing Medicare Medicaid 2026 options.
Projected 2026 Medicaid Updates
The future of Medicaid in 2026 will largely depend on federal policy decisions and state budget priorities. There could be continued discussions around block grants or per capita caps, which would fundamentally alter federal funding for the program and potentially lead to changes in state-level benefits and eligibility. States are also likely to continue exploring managed care models to improve efficiency and care coordination. Beneficiaries and potential applicants should remain vigilant about state-specific proposals and legislative actions that could impact their coverage. The dynamic nature of Medicaid, especially in the context of Medicare Medicaid 2026, requires continuous monitoring of local and federal policy developments.
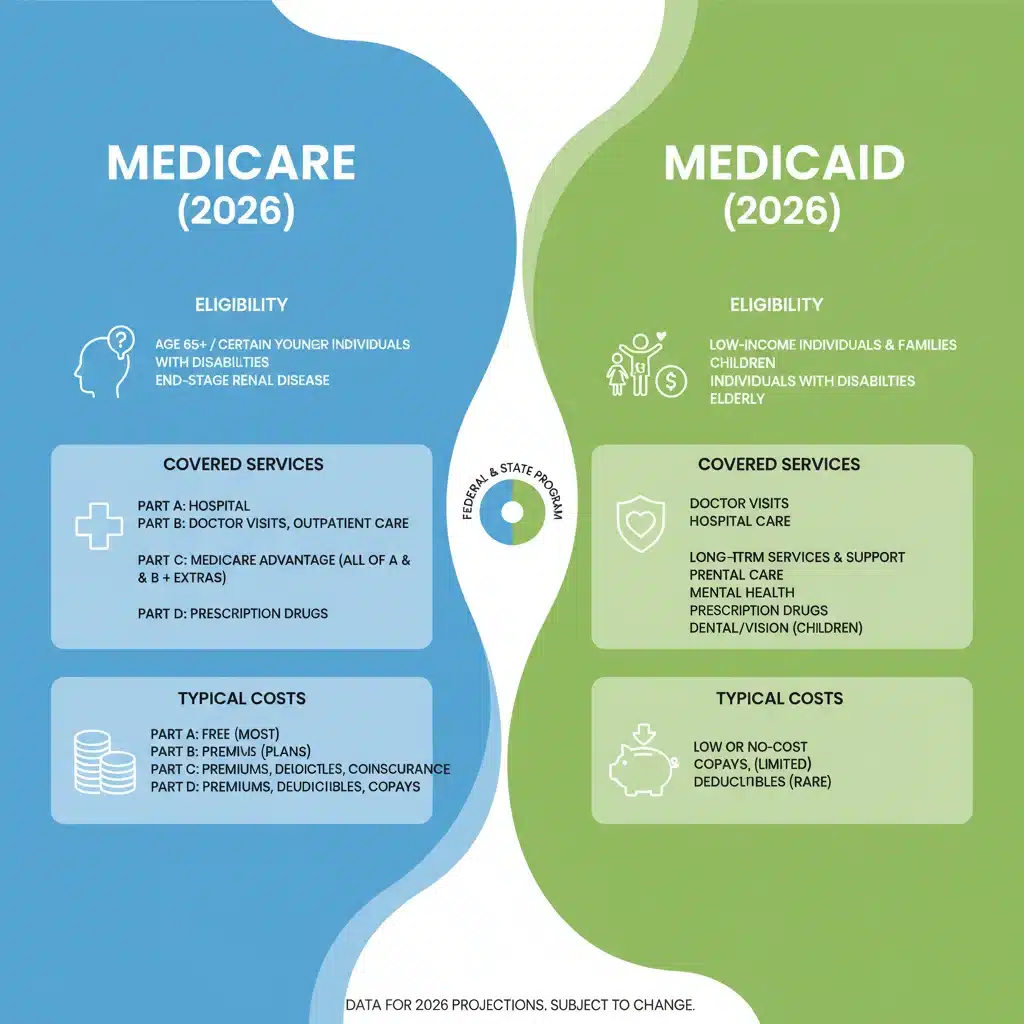
Key Differences and Overlaps: Medicare vs. Medicaid
While both programs provide essential healthcare, understanding their fundamental distinctions is vital for making informed decisions. The primary differentiator lies in their target populations and funding mechanisms, leading to variations in eligibility, benefits, and cost structures.
Eligibility: Age vs. Income
- Medicare: Primarily age-based (65+), or disability-based (after a qualifying period) or specific diseases (ESRD, ALS), regardless of income.
- Medicaid: Primarily income-based for low-income individuals and families, with varying thresholds by state and specific population groups (e.g., children, pregnant women, adults, people with disabilities).
Benefits and Services
- Medicare: Covers hospital stays, doctor visits, outpatient care, preventive services, and (optionally) prescription drugs and additional benefits through Advantage plans. It does not typically cover long-term custodial care.
- Medicaid: Offers comprehensive benefits, including doctor visits, hospital stays, prescription drugs, mental health services, and significantly, often covers long-term care services, including nursing home care and home-based care, which is a critical distinction for many elderly and disabled individuals.
Costs and Premiums
- Medicare: Most beneficiaries pay premiums for Part B and Part D, along with deductibles and co-insurance. There are varying out-of-pocket costs depending on the plan type (Original Medicare vs. Medicare Advantage).
- Medicaid: Generally, beneficiaries pay very little or no out-of-pocket costs, including premiums, deductibles, and co-payments, although some states may impose nominal co-pays for certain services.
Administration
- Medicare: A federal program administered by the Centers for Medicare & Medicaid Services (CMS).
- Medicaid: A joint federal and state program, with states having significant flexibility in designing and administering their specific programs within federal guidelines.
These distinctions are crucial when considering your healthcare options for Medicare Medicaid 2026. For instance, an individual who is 65 but has a very low income might qualify for both programs, leading to a dual-eligible status.
Dual Eligibility: When Medicare and Medicaid Work Together for 2026
Many individuals find themselves in a unique position where they qualify for both Medicare and Medicaid. These individuals are known as "dual eligibles." When you have both Medicare and Medicaid, the two programs work together to cover your healthcare costs, often resulting in minimal or no out-of-pocket expenses for the beneficiary. This is a powerful combination for those who meet the criteria, particularly as we look towards Medicare Medicaid 2026 updates.
How Dual Eligibility Works
For dual eligibles, Medicare is generally the primary payer for Medicare-covered services. This means Medicare pays first. Medicaid then acts as the secondary payer, covering costs that Medicare doesn’t, such as Medicare premiums (Part A if applicable, Part B, and sometimes Part D), deductibles, co-insurance, and co-payments. Additionally, Medicaid may cover services that Medicare does not, such as long-term care services and supports, which is a significant benefit for many seniors and individuals with disabilities. This coordination significantly reduces the financial burden on beneficiaries, providing a more comprehensive safety net.
Types of Dual Eligibility
There are different categories of dual eligibles, each with varying levels of Medicaid assistance:
- Full-Benefit Dual Eligibles: These individuals receive the full range of Medicare and Medicaid benefits. Medicaid covers their Medicare premiums, deductibles, co-insurance, and co-payments, as well as services not covered by Medicare.
- Partial-Benefit Dual Eligibles (Medicare Savings Programs – MSPs): These individuals receive help from Medicaid to pay for some of their Medicare costs, such as premiums, deductibles, and co-insurance, but do not receive full Medicaid benefits. There are several types of MSPs, including:
- Qualified Medicare Beneficiary (QMB) Program: Helps pay for Part A and Part B premiums, deductibles, and co-insurance.
- Specified Low-Income Medicare Beneficiary (SLMB) Program: Helps pay for Part B premiums only.
- Qualifying Individual (QI) Program: Helps pay for Part B premiums only, with slightly higher income limits than SLMB.
- Qualified Disabled and Working Individuals (QDWI) Program: Helps pay for Part A premiums for certain disabled individuals who lost their premium-free Part A when they returned to work.
Benefits of Dual Eligibility for 2026
For individuals eligible for both programs, the advantages are substantial. It provides access to a much broader range of healthcare services with significantly reduced out-of-pocket costs. This can be particularly beneficial for those with chronic conditions or those requiring extensive medical care, including long-term care. As we approach 2026, understanding how these programs coordinate will be essential for maximizing healthcare benefits and minimizing financial strain. The synergy of Medicare Medicaid 2026 provides a robust solution for many vulnerable populations.
Navigating Enrollment and Application for 2026
Enrolling in Medicare or applying for Medicaid can seem complex, but understanding the general process for 2026 can simplify your journey. While Medicare enrollment is primarily managed federally, Medicaid applications are handled at the state level.
Medicare Enrollment for 2026
For most people, Medicare enrollment is automatic if they are already receiving Social Security or Railroad Retirement Board benefits when they turn 65. Otherwise, individuals need to actively enroll.
- Initial Enrollment Period (IEP): This is a 7-month window that begins 3 months before your 65th birthday month, includes your birthday month, and extends 3 months after. It’s crucial to enroll during this period to avoid potential late enrollment penalties for Part B and Part D.
- General Enrollment Period (GEP): If you miss your IEP, you can enroll during the GEP, which is from January 1 to March 31 each year. Coverage would then begin on July 1.
- Special Enrollment Period (SEP): If you delay enrollment due to certain circumstances (e.g., still working and covered by an employer health plan), you might qualify for an SEP.
- Annual Enrollment Period (AEP): From October 15 to December 7 each year, individuals can make changes to their Medicare Advantage and Part D plans. This is a critical time to review Medicare Medicaid 2026 plan options.
For 2026, it’s always advisable to check the official Medicare website or contact them directly for the most up-to-date enrollment deadlines and requirements, as minor adjustments can occur.
Medicaid Application for 2026
Applying for Medicaid is done through your state’s Medicaid agency or through the Health Insurance Marketplace (healthcare.gov). The process typically involves:
- Gathering Documentation: You’ll need proof of income, household size, residency, and citizenship or lawful immigration status.
- Submitting an Application: This can usually be done online, by mail, or in person.
- Verification Process: The state agency will review your application and documentation to determine eligibility.
Given that Medicaid rules vary by state, it’s imperative to consult your state’s specific Medicaid website or contact their office directly for detailed information on eligibility and the application process for 2026. States may update their application portals or require new forms, making timely information crucial for prospective beneficiaries of Medicare Medicaid 2026.

Anticipated Policy Changes and Future Outlook for 2026
The healthcare landscape is constantly evolving, and 2026 is expected to bring its share of policy discussions and potential reforms for both Medicare and Medicaid. Understanding these anticipated changes is crucial for anyone relying on or planning to rely on these programs.
Medicare Policy Discussions
For Medicare, ongoing debates typically center around:
- Program Solvency: Discussions about the long-term financial health of the Medicare trust fund are perennial. Policymakers may explore options such as adjusting eligibility ages, increasing revenues, or modifying benefit structures. Any significant changes would likely be phased in over several years, but the groundwork for 2026 could be laid now.
- Prescription Drug Costs: The Inflation Reduction Act of 2022 introduced significant changes to Medicare Part D, including drug price negotiation and capping out-of-pocket costs for beneficiaries. 2026 will see further implementation of these provisions, with more drugs becoming eligible for negotiation, potentially leading to lower costs for beneficiaries.
- Telehealth Expansion: The increased use of telehealth services, spurred by the pandemic, is likely to continue being integrated into Medicare policy. Expect discussions on permanent reimbursement for a broader range of telehealth services, enhancing access to care, particularly in rural areas.
- Medicare Advantage Oversight: With the growth of Medicare Advantage plans, there’s ongoing scrutiny regarding their quality, marketing practices, and payment models. Future policies in 2026 might focus on ensuring plans provide adequate access to care and operate transparently.
Medicaid Policy Discussions
Medicaid’s future is closely tied to federal and state budgets and philosophical approaches to safety net programs:
- Federal Funding Structure: Proposals for block grants or per capita caps for federal Medicaid funding could resurface. If enacted, these would give states more flexibility but could also lead to reduced benefits or stricter eligibility in some states, depending on their financial capacity and priorities.
- Medicaid Expansion: The political landscape around Medicaid expansion under the ACA continues to shift. More states might consider expansion, or existing expansion states could face new challenges based on federal policy. This directly impacts the number of low-income adults covered.
- Home and Community-Based Services (HCBS): There’s a growing emphasis on HCBS to allow individuals to receive care in their homes and communities rather than institutions. 2026 could see increased funding or policy directives to expand access to these services, which are crucial for many elderly and disabled Medicaid beneficiaries.
- Addressing Health Disparities: Both federal and state governments are increasingly focusing on using Medicaid to address health disparities and promote health equity, potentially through targeted programs and outreach initiatives.
Staying informed about these policy discussions is vital for understanding the potential evolution of Medicare Medicaid 2026. Advocacy groups, government websites, and reputable news sources will be key resources for tracking these developments.
Choosing the Right Path: Making Informed Decisions for 2026
Deciding between Medicare, Medicaid, or understanding how they can work together requires careful consideration of your personal circumstances. There is no one-size-fits-all answer, and what works best for one individual may not be suitable for another.
Self-Assessment Questions:
- Are you 65 or older, or do you have a qualifying disability or medical condition? If so, Medicare is likely your primary consideration.
- What is your income and household size? If you have limited income and resources, Medicaid could provide comprehensive, low-cost coverage.
- Do you anticipate needing long-term care services? Medicaid is a significant payer for long-term care, whereas Medicare generally is not.
- What are your prescription drug needs? Both Medicare Part D and Medicaid offer drug coverage, but their formularies and costs differ.
- Are you eligible for both programs? If so, understanding the benefits of dual eligibility can dramatically reduce your healthcare costs.
Resources for Assistance:
Navigating the complexities of Medicare Medicaid 2026 doesn’t have to be a solitary endeavor. Several resources are available to help you make informed decisions:
- State Health Insurance Assistance Programs (SHIPs): These programs offer free, unbiased counseling to Medicare beneficiaries and their families. They can help you understand your options, compare plans, and apply for assistance programs.
- Medicaid Agencies: Your state’s Medicaid office can provide detailed information on eligibility, application processes, and covered benefits specific to your state.
- Social Security Administration (SSA): The SSA handles Medicare enrollment for most individuals and can provide information on eligibility and benefit payments.
- Official Government Websites: Medicare.gov and Medicaid.gov are invaluable resources for the latest information, fact sheets, and tools.
- Healthcare Navigators: These individuals or organizations provide free assistance to help consumers understand their health insurance options and enroll in coverage through the Health Insurance Marketplace, which can include Medicaid.
Proactive research and seeking expert advice are the best ways to ensure you have the appropriate healthcare coverage for 2026. The landscape of Medicare Medicaid 2026 is complex, but with the right information and support, you can confidently choose the path that best meets your healthcare and financial needs.
Conclusion: Securing Your Health Coverage in 2026
The journey through the American healthcare system can be intricate, particularly when distinguishing between programs as vital and expansive as Medicare and Medicaid. As we have explored, while both serve to provide essential health coverage, they cater to distinct populations through different mechanisms. Medicare is primarily an age- or disability-based federal entitlement program, offering various parts (A, B, C, D) to cover hospital, medical, and prescription drug needs. Medicaid, on the other hand, is a needs-based, joint federal-state program designed for low-income individuals and families, providing comprehensive benefits that often include crucial long-term care services.
The anticipated updates and policy discussions for Medicare Medicaid 2026 underscore the dynamic nature of these programs. Potential changes in premiums, deductibles, drug pricing, eligibility thresholds, and service offerings mean that continuous vigilance and proactive research are paramount. For those who are dual-eligible, the synergistic relationship between Medicare and Medicaid offers a powerful safety net, significantly reducing out-of-pocket costs and expanding access to necessary care.
Making an informed decision about your healthcare coverage for 2026 requires understanding your personal circumstances, including your age, income, health status, and specific medical needs. Utilizing the available resources, such as SHIPs, state Medicaid agencies, and official government websites, will empower you to navigate the complexities and select the most appropriate coverage. Whether you are aging into Medicare, managing a disability, or seeking assistance for low-income healthcare, a clear understanding of Medicare Medicaid 2026 is not just beneficial, but essential for securing your health and financial well-being in the coming years. Plan ahead, stay informed, and advocate for your healthcare needs to ensure you receive the best possible coverage.





